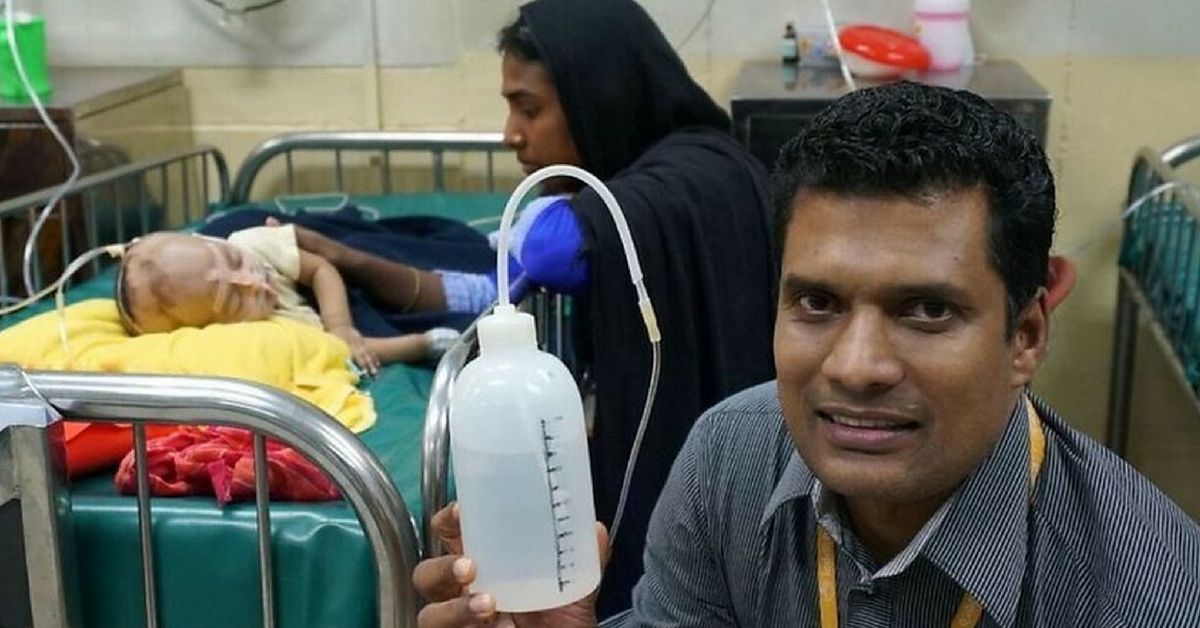
The first night on the job, working in the pediatric department, he watched three children die right before his eyes. That night he made a promise to do something to stop children from dying of pneumonia.
Dr. Mohammod Jobayer Chisti vowed to change the world of medicine that night in 1996, and he has done it.
About 920,000 babies and small children pass away each year from pneumonia in South Asia and Sub-Saharan Africa. After two decades of research, the father-of-three has come up with a low-cost device that has the potential to save thousands of babies' lives.

Pneumonia is a illness that affects the lungs after infections from bacteria or a virus. The lungs become swollen and fill with fluid which reduces the patient's ability to breathe.
In developed countries hospitals use ventilators to help people suffering from pneumonia to breathe. Each machine, however, costs up to $15,000 and must have specially-trained staff operate the ventilator. This makes them too expensive for some hospitals in some developing countries.
The World Health Organization recommends a lower-cost alternative of using a low-flow oxygen machine, but it still results in one in seven children dying.
While Dr. Christi was working in Melbourne, Australia, he got inspiration for a better solution that would save more lives.
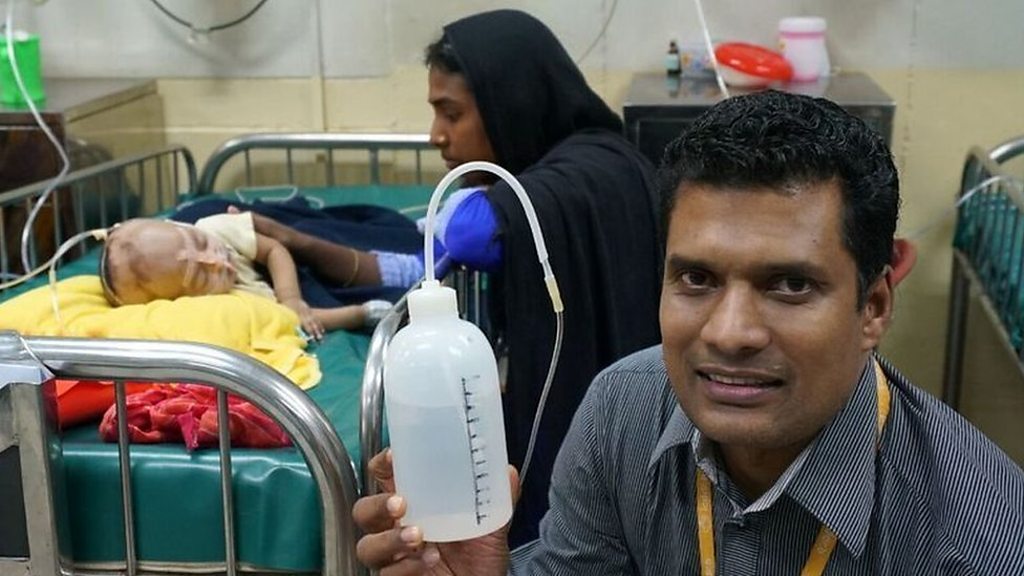
The machine that inspired Dr. Christi uses continuous positive airway pressure (CPAP) to prevent lungs from collapsing, it helps the body to absorb enough oxygen. This machine, of course, came with a mighty price tag.
When he returned home, he got to work on a cheaper version of the CPAP device. He and a colleague got an empty shampoo bottle from the intensive care unit and filled it with water. They inserted one end of the plastic supply tubing into the bottle.
"The children inhale oxygen from a tank and exhale through a tube which is inserted into a bottle of water producing bubbles in the water," Dr. Chisti explains.
The pressure from the bubbles keeps the small air sacs of the lungs open.
"We tested it on four or five patients at random. We saw a significant improvement within a few hours," he said.
This included Kohinoor Begum's daughter.

After a two year study, Dr. Christi shared the results and it showed that children who were treated with the bubble CPAP device had a much better chance of survival than those who were treated with the low-flow oxygen.
At at cost of just $1.25 each, the device appears to have cut mortality rates by 75%.
Since the device has also created a more efficient use of oxygen, it has saved the hospital $24,000 annually, slashing the yearly bill from $30,000 to just $6,000.
"I think this innovation has great potential to reduce the mortality rate drastically because any hospital can afford this," Dr. ARM Luthful Kabir, professor of paediatrics at Ad-din Women's Medical College says.
So far 600 children have benefited from this low-cost device and Dr. Christi has been promoted to the head of clinical research at his hospital.
Finally fulfilling a promise he made twenty years earlier, Dr. Christi says, "I have no language to express this."
Source: BBC