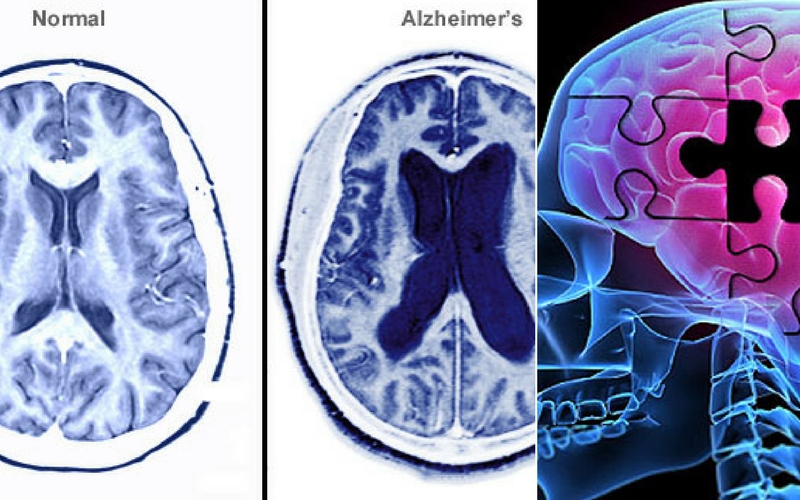
The number of scientists claiming that depression is a result of chronic inflammation is on the rise, and apparently, inflammation has a huge impact on mental health.
Psychoneuroimmunology is the study of these links, which analyzed the effects of inflammation on behavior. The journal Neuropsychopharmacology published a 2012 study which found that:
"Elevated biomarkers of inflammation, including inflammatory cytokines and acute-phase proteins, have been found in depressed patients, and administration of inflammatory stimuli has been associated with the development of depressive symptoms.
Data also have demonstrated that inflammatory cytokines can interact with multiple pathways known to be involved in the development of depression, including monoamine metabolism, neuroendocrine function, synaptic plasticity, and neurocircuits relevant to mood regulation ...
Psychosocial stress, diet, obesity, a leaky gut and an imbalance between regulatory and pro-inflammatory T cells also contribute to inflammation and may serve as a focus for preventative strategies relevant to both the development of depression and its recurrence."
These studies regard depression as a result of the attempts of the body to fight the inflammatory response and to involve hormones and neurotransmitters. The most common symptoms of depression linked to inflammation include metabolic changes, mood changes, avoidance, slowed thinking, and alterations in perception.
Cytokines in the blood or inflammatory messengers like CRP, interleukin-1 (IL-1), TNF-alpha, and interleukin-6 (IL-6) are predictive of and correlate to depression.
For instance, in the case of bipolar disorders, melancholic depression, and postpartum depression, white blood cells known as monocytes express pro-inflammatory genes that trigger the release of cytokines, while the cortisol sensitivity is reduced. These inflammatory agents stimulate the vagus nerve that links the brain and gut and thus transfer information to the nervous system.
Inflammation activates the brain cells known as microglia, and the enzyme indoleamine 2 3-dioxygenase (IDO) directs tryptophan away from the melatonin and serotonin production, triggering the production of NMDA (an amino acid derivative) agonist known as quinolinic acid, which causes anxiety and agitation.
Researchers have recently highlighted the inflammatory underpinnings of depression, and BBC reported:
"The focus is on an errant immune system causing inflammation in the body and altering mood ... [Professor Ed Bullmore, Ph.D., head of psychiatry at the University of Cambridge and an employee of GlaxoSmithKline] said: "˜Depression and inflammation often go hand in hand ...
[I]f you have flu, the immune system reacts to that, you become inflamed and very often people find that their mood changes too. Their [behavior] changes, they may become less sociable, more sleepy [and] more withdrawn.
They may begin to have some of the negative ways of thinking that are characteristic of depression and all of that follows an infection' ...
Inflammation is part of the immune system's response to danger ... If it is too high, it causes damage. And for some reason, about one-third of depressed patients have consistently high levels of inflammation."
When patients suffering from rheumatoid arthritis were prescribed to use anti-inflammatory drugs to boost specific parts of the immune system, they reported too, so professor Iain McInnes, a consultant rheumatologist, told the BBC:
"When we give these therapies we see a fairly rapid increase in a sense of well-being, mood state improving quite remarkably often disproportionately given the amount of inflammation we can see in their joints and their skin."
His team conducted brain scans on patients diagnosed with rheumatoid arthritis, before and after receiving an immune targeted drug, and the results of the scans confirmed the feedback of the patients. The use of the drug greatly changed the neurochemical circuitry of the brain and beneficially affected the pathways involved in alleviating depression.
Moreover, Carmine Pariante, a professor of biological psychiatry, found that individuals with overactive immune systems are less likely to respond to anti-depressants. Emotional trauma might change the immune system in a way that it will make one prone to depression. Pariante says:
"We think the immune system is the key mechanism by which early life events produce this long-term effect.
We have some data showing adult individuals who have a history of early life trauma, even if they have never been depressed, have an activated immune system so they are in a state of risk."
Currently, researchers are testing the arthritis drug sirukumab on depressed patients. Yet, this approach will just switch the focus from one drug to another, and all drugs cause severe side-effects.
However, drugs are not the only way to fight inflammation. Fortunately, you can combat it in a completely natural way.
One of the most effective methods involves a ketogenic diet, which is rich in healthy fats and low in net carbs (total carbs minus fiber). The nutritional ketosis drives the inflammation levels extremely low, and it virtually makes the C-reactive protein (CRP) level (an inflammatory marker) disappear.
Nuts Fight Inflammation
Raw nuts are abundant in healthy fat, and researchers have found that the consumption of 1 ounce (about a handful) of nuts five times weekly lowers inflammation. Reuters reported:
"Past research has linked eating nuts to lower rates of heart disease and diabetes, but the exact reason was unknown, senior study author Dr. Ying Bao, an assistant professor of medicine at Harvard Medical School in Boston, told Reuters Health. "˜We hypothesized that nuts may exert these health benefits by reducing inflammation,' Bao said ..."
Two long-term studies "” the Nurses' Health Study (NHS) and the Health Professionals Follow-Up Study (HPFS) "” analyzed the diet of participants and took their blood samples for inflammatory biomarkers.
The findings showed that the ones who consumed nuts at least five times a week had 20 percent lower CRP levels and 16 percent lower IL-6.
The results were the same even when researchers took other anti-inflammatory dietary and lifestyle strategies into account, including body weight, smoking, and exercise. The regular consumption of nuts offers numerous health benefits, such as:
- Improved heart health
- Weight loss
- Lower risk of metabolic syndrome and diabetes
- Lower systolic blood pressure
- Lower mortality risk and increased longevity( Researchers found that individuals who ate a small handful (1 ounce or 28 grams) of nuts daily were 20 percent less likely to die for any reason. Studies found that the consumption of nuts at least 5 times per week led to a 29 percent drop in mortality risk from heart disease, and a lower mortality risk from cancer by 11%.
Anti-inflammatory ingredients in nuts include antioxidants, fiber, magnesium, the amino acid L-arginine and unsaturated fatty acids like α-linolenic acid.
Processing destroys many of the nutrients in nuts, while the antioxidants are mostly concentrated in the skin, so make sure you consume raw, organic, and unpeeled nuts.
Macadamia and pecans are the highest in healthy fats, and lowest in carbs and protein. Raw macadamia nuts are also high in manganese, magnesium, and vitamin B, and 60 percent of the fatty acid in macadamia is the beneficial monounsaturated fat oleic acid.
One ounce of macadamia nuts contains 4 grams of carbs, but more than a half of those are non-digestible fiber, so it provides an ultra-low 2 grams of sugar per ounce of nuts.
Pecans contain over 19 different vitamins and minerals that improve the health of the arteries and lower LDL cholesterol and are listed among the top 15 foods known for their antioxidant activity, according to the U.S. Department of Agriculture (USDA).
One of these antioxidants is vitamin e, which supports the neurological health and prevents the oxidation of blood lipids. Pecans are also full of lutein, beta-carotene, and zeaxanthin, which fight inflammation and prevent free radical damage.
Furthermore, animal-based omega-3 is a powerful anti-inflammatory, and it can be found in many nuts. However, our body finds it hard to turn the alpha-linolenic acid (ALA) found in plants into the docosahexaenoic acid (DHA) found in marine animals like fatty fish and krill. DHA is essential for the health of the brain since 90% of the omega-3 fat in the brain tissue is DHA.
Also, the marine-based DHA and eicosapentaenoic acid (EPA) are structural elements important for every single body cell, so it is of high importance to remember that you cannot obtain all the needed omega-3 from plant sources.
Rich sources of animal-based DHA and EPA include fatty, cold-water fish such as sardines, fish roe, wild Alaskan salmon, herring, and krill oil.
Inflammation is also fought by vitamin D, and this vitamin is best obtained from sensible sun exposure. It causes the production of more than 200 anti-microbial peptides and up-regulates numerous genes, including the one that helps the body to fight chronic inflammation and infections.
The findings of a placebo-controlled study indicate that the high doses of vitamin D supplementation improved anti-inflammatory molecules, and can be used as an anti-inflammatory "medicine" in the case of heart failure.
The results showed that the daily dose of 50 micrograms (mcg) of vitamin D taken within a period of 9 months elevated blood concentrations of anti-inflammatory interleukin-10 (IL-10) by 43 percent, and prevented the rise of the levels of the pro-inflammatory cytokine TNF-alpha in patients diagnosed with congestive heart failure (CHF).
Studies have also found a link between vitamin D deficiency and depression. Namely, seniors with the lowest levels of vitamin D had an 11 times higher risk to become depressed than the ones with normal levels.
The brain tissue has various vitamin D receptors, and the optimal levels of this vitamin improve some essential chemicals in the body and protect brain cells by boosting the effectiveness of glial cells.
You can also take vitamin D3 supplements, but you need to monitor your levels on a regular basis. The levels in your body need to be at least 40 to 60 nanograms per milliliter (ng/ml).
However, note that the oral supplementation of vitamin D3 has its inherent dangers, as it is a hormone and has important physiologic actions.
Our body is designed to get almost all of our vitamin D from solar exposure and vitamin D is a marker for UV light exposure, which has its metabolic benefits. The oral supplementation might send a false signal which might disrupt some important physiological cycles. To treat depression, you need all the frequencies.
For instance, daily exposure to sunlight outdoors without glasses or contacts for a few minutes within an hour is a potent stimulus that normalizes the circadian rhythm and improves sleep, which helps in the case of depression.
To sum up, in order to treat inflammation, it is of utmost importance to consume a healthy diet and increase the intake of animal-based omega-3 and vitamin D.
Avoid all kinds of processed foods, and turn to real foods, rich in nutrients and antioxidants that fight inflammation. Increase the intake of nuts, as rich sources of healthy fats.
You should consider a ketogenic diet, which offers incredible benefits.
Moreover, depression can be caused by the impaired gut flora, so increase the intake of fermented and cultured foods, like natto, kefir, kimchi and fermented vegetables.
The post Why The Link Between Depression and Inflammation Should Not Be Ignored Any Longer appeared first on Healthy Life Box.